24 Mar 2023 Tuberculosis
Tuberculosis
Common symptoms of active lung Tuberculosis are cough with sputum and blood at times, chest pains, weakness, weight loss, fever, and night sweats. WHO recommends the use of rapid molecular diagnostic tests as the initial diagnostic test in all persons with signs and symptoms of Tuberculosis as they have high diagnostic accuracy and will lead to major improvements in the early detection of Tuberculosis and drug-resistant Tuberculosis. Rapid tests recommended by WHO are the Xpert MTuberculosis/RIF Ultra and Truenat assays.
Diagnosing multidrug-resistant and other resistant forms of Tuberculosis (see Multidrug-resistant Tuberculosis section below) as well as HIV-associated Tuberculosis can be complex and expensive.
Tuberculosis is particularly difficult to diagnose in children.
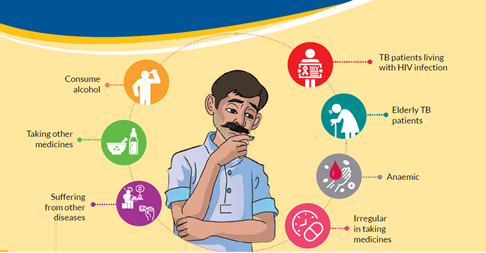
Tuberculosis
Treatment of Tuberculosis
- Tuberculosis is a treatable and curable disease. Drug-susceptible Tuberculosis disease is treated with a standard 4-month or 6-month course of 4 antimicrobial drugs that are provided with support to the patient by a health worker or trained treatment supporter. Without such support, treatment adherence is more difficult.
- Since 2000, an estimated 74 million lives were saved through Tuberculosis diagnosis and treatment.
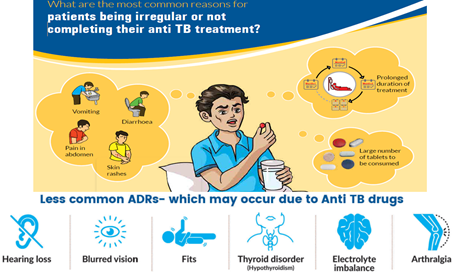
TB treatment
Multidrug of Tuberculosis(MDR-TB)
- Tuberculosis medicines have been used for decades and strains that are resistant to one or more of the medicines have been documented in every country surveyed.
- Drug resistance emerges when Tuberculosis medicines are used inappropriately, through incorrect prescription by health care providers, poor quality drugs, and patients stopping treatment prematurely.
- Multidrug-resistant tuberculosis (MDR-Tuberculosis) is a form of Tuberculosis caused by bacteria that do not respond to isoniazid and rifampicin, the 2 most effective first-line Tuberculosis drugs.
- MDR-Tuberculosis is treatable and curable by using second-line drugs. However, second-line treatment options are limited and require extensive chemotherapy (of at least 9 months and up to 20 months of treatment) with medicines that are expensive and toxic.
- In some cases, more extensive drug resistance can develop. Tuberculosis caused by bacteria that do not respond to the most effective second-line Tuberculosis drugs can leave patients with limited treatment options.
- MDR-Tuberculosis remains a public health crisis and a health security threat.
- In accordance with WHO guidelines, detection of MDR/RR-Tuberculosis requires bacteriological confirmation of Tuberculosis and testing for drug resistance using rapid molecular tests, culture methods or sequencing technologies.
- Treatment of MDR/RR-Tuberculosis requires a course of second-line drugs for at least 9 months and up to 20 months, supported by counselling and monitoring for adverse events. WHO recommends expanded access to all-oral regimens.
- Only about one in three people with drug resistant Tuberculosis accessed treatment in 2020.
- Worldwide in 2019, the treatment success rate of MDR/RR-Tuberculosis patients was 60%. In 2020, WHO recommended a new shorter (9–11 months) and full oral regimen for patients with MDB-Tuberculosis.
- Research findings have shown that patients find it easier to complete the regimen, compared with the longer regimens that last up to 20 months. Resistance to fluoroquinolones should be excluded prior to the initiation of treatment with this regimen.
- By the end of 2021, 92 countries started using shorter MDR-Tuberculosis treatment regimens and 109 had started using bedaquiline, in an effort to improve the effectiveness of MDR-TB treatment.
India’s status in Tuberculosis
- The government’s National Tuberculosis Elimination Program collects the majority of India’s TB statistics.
- According to WHO, An estimated 2.8 million TB cases with TB killing more than 4,00,000 occur in India every year.
Measures were taken by India to eradicate Tuberculosis
- The National Tuberculosis Elimination Programme(NTEP): It aims to reduce India’s tuberculosis burden by 2025 strategically.
- The National Strategic Plan for TB Elimination:
- Its multi-pronged approach aimed to detect all TB patients, with a focus on Tuberculosis patients seeking care from private providers and undiagnosed Tuberculosis, and was launched in a mission mode to meet the target of eradicating Tuberculosis by 2025.
- Ni-Akshay Poshan Yojana(NPY)(Nutritional Support to TB): It contributes to meeting the dietary needs of TB patients, particularly those who are underserved.
- From 2018 to the present, about Rs. 1,707 crores has been disbursed to over 65 lakh patients undergoing TB treatment across the country.
- Patient-Provider Support Agencies (PPSA): Patient Provider Support Agencies (PPSA) have been rolled out in 250 districts through the domestic setup and JEET program to engage the commercial sector.
- Universal Drug Susceptibility Testing (UDST): To ensure that every diagnosed TB patient is tested for medication resistance prior to or at the time of treatment beginning.
- Pradhan Mantri TB Mukt Bharat Abhiyaan: To bring all community stakeholders together to help persons receiving TB treatment and to expedite the country’s progress towards TB elimination.
- Ayushman Bharat – Health and Wellness Centres: Decentralize comprehensive primary care, including tuberculosis care, at the grassroots level.
- Bedaquiline and Delamanid: Newer medications, such as bedaquiline and delamanid, have also been approved for the treatment of DRTB.
Need of the hour:
- The development and widespread use of an adult tuberculosis vaccination.
- Reduce production costs so that fewer anti-TB medications are available to everyone
- Developing injection-free and oral TB medications
- For diagnosing tuberculosis, AI-assisted portable radiography with 90-second reporting and 95% accuracy is used.
Source:
Get Current Affairs from Yojna IAS


No Comments